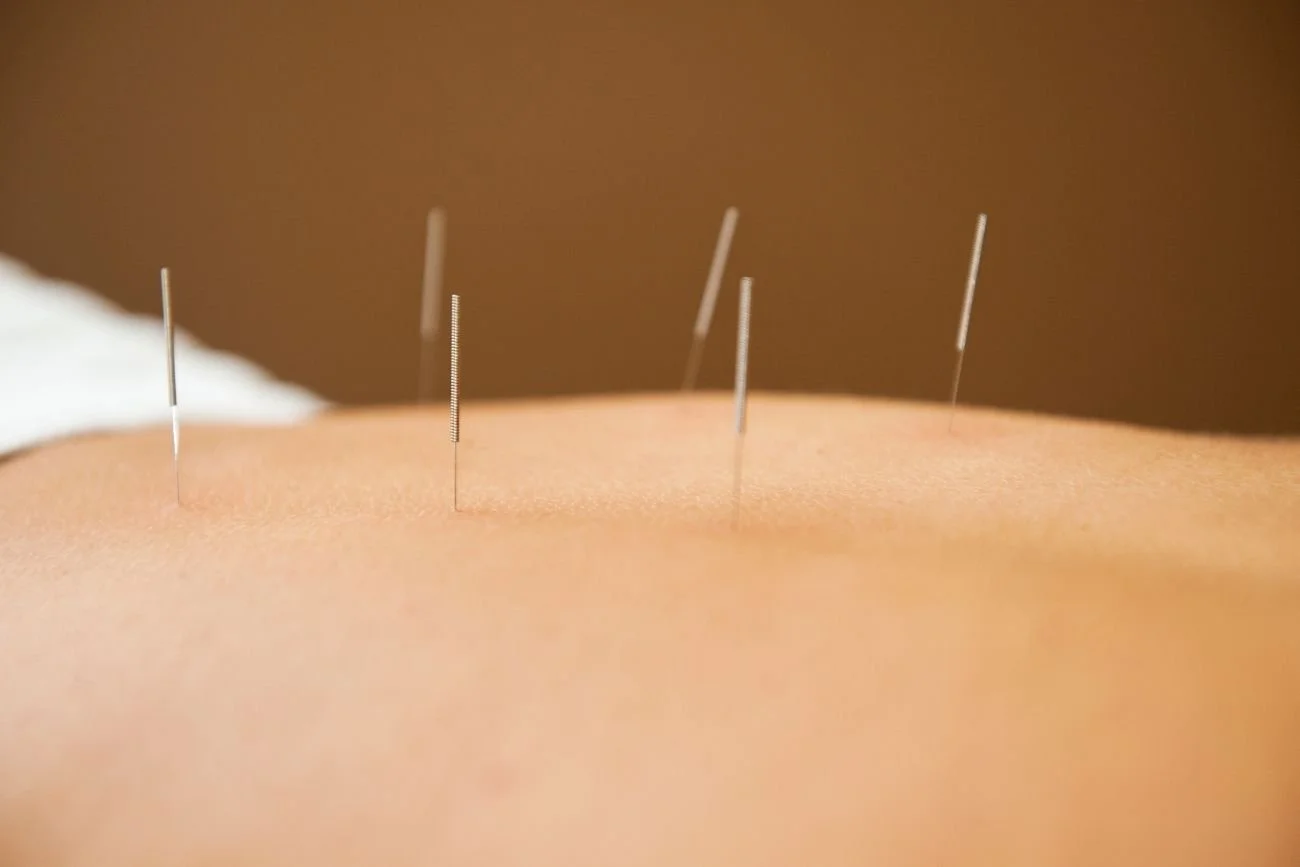
Living with POTS: Finding Treatment That Supports You
You might look fine on the outside, but what’s happening inside your body can feel like a full-blown storm.
This post is for people living with Postural Orthostatic Tachycardia Syndrome (POTS) who want a clearer understanding of treatment options, including where acupuncture may fit as a non-invasive, supportive approach.
POTS isn’t just “being dizzy” or “feeling tired.” It can look like standing up and suddenly hearing your heartbeat in your ears. Reaching for a glass of water and realizing your hands are shaking. Watching your vision go gray at the edges while you try to stay present in a conversation at work.
It’s the frustration of being told to “just push through” when pushing through often makes symptoms worse.
For many people living with POTS, daily life becomes a series of exhausting calculations:
- How long can I stand before I feel faint?
- Will I have enough energy to shower and make a meal today?
- How do I explain to my boss again why I need to sit down right now?
And beneath the physical symptoms, there’s something even more depleting: the emotional toll of not being believed.
Especially for teenagers and young women, who are most commonly affected by POTS, symptoms are often dismissed or misdiagnosed as anxiety or stress.2 Pediatric patients are frequently described as high-achieving, healthy adolescents who become ill after an infection or growth spurt and don’t bounce back the way others do.1 These are the “ideal kids” who suddenly struggle to get out of bed, attend school, or even walk across a room without getting dizzy.
You may have been told it’s “all in your head,” or that you’re just sensitive or lazy. But what you’re living with is real, and it has a neurological basis. POTS is a disorder of the autonomic nervous system, the part of the body responsible for regulating heart rate, blood pressure, and digestion. In people with POTS, that system can become dysfunctional, leading to an exaggerated increase in heart rate when moving from lying down to standing.2
There’s grief in this, too: grieving the life you had before your body changed. Maybe you were athletic. Maybe you had a social life you loved, or a career you were building. And now even simple things, like walking the dog, standing in line, or taking a shower, can leave you drained.
POTS is often invisible to others, but its impact can be life-altering. While estimates vary, it’s believed that 1 to 3 million people in the United States may be living with POTS, many without a proper diagnosis.3 The condition is still widely underrecognized, even among physicians, and delays in diagnosis can add to the burden patients carry.3
If POTS has made your world feel smaller, you’re not alone. With the right evaluation and a structured plan, many people find strategies that improve day-to-day function and quality of life, including approaches that support nervous system regulation over time.
What Is POTS, and Why Does It Affect So Many Areas of Life?
POTS stands for Postural Orthostatic Tachycardia Syndrome, but the name doesn’t capture the day-to-day reality of living with it.
POTS is a form of dysautonomia, meaning the autonomic nervous system isn’t regulating as smoothly as it should. This system controls functions your body normally manages automatically, including heart rate, blood pressure, digestion, and temperature. When you have POTS, symptoms often intensify when you move from lying down to standing. A hallmark feature is a rapid rise in heart rate, often 30 beats per minute or more within 10 minutes of standing, even without a drop in blood pressure.2
What that feels like can vary, but many people describe symptoms such as:
- Lightheadedness or near-fainting when standing
- A pounding or racing heart
- Severe fatigue and post-exertional crashes
- Nausea or “tummy upset” after eating
- Brain fog and difficulty concentrating
- Cold hands and feet
- Exercise intolerance or full-body exhaustion after basic activity
Some people experience several symptoms at once. Others cycle through flares that can feel unpredictable and make it hard to trust how their body will respond from one hour to the next.
Many patients are first told these symptoms are due to dehydration, anxiety, or simply being “out of shape.” But these experiences can reflect measurable changes in circulation and nervous system signaling that are identifiable when clinicians know what to assess.3
There are different types of POTS, including:
- Neuropathic POTS, where there’s damage or dysfunction in the small nerve fibers that help control blood vessel tone
- Hyperadrenergic POTS, where the body produces too much norepinephrine (a stress hormone), leading to feelings of panic or surges in heart rate
- Secondary POTS, which develops in connection with another condition like Ehlers-Danlos Syndrome (EDS) (a connective tissue condition often associated with hypermobility), Lyme disease, or a viral illness like COVID-192
Although POTS can affect anyone, it is most common in females between the ages of 15 and 50, and it often begins during adolescence, especially after a period of rapid growth, hormonal shifts, or recovery from an illness.1 This is one reason many pediatric patients are misdiagnosed or brushed off early on, particularly if they “look fine” on the outside.1
The impact can be significant. For young adults, POTS may mean missing school, losing momentum, or watching friendships slip away while it takes everything they have just to get through the day. For working adults, it can contribute to job instability, financial strain, and a gradual loss of confidence in their body and mind.3
Despite being recognized by the medical community for over a decade, POTS is still frequently underdiagnosed, and patients often see multiple doctors over several years before receiving an accurate diagnosis.3 That delay can prolong suffering and erode trust in the healthcare system, leaving many people feeling discouraged before they’ve even been given a clear plan forward.
Why Typical POTS Treatments Often Fall Short
By the time a diagnosis arrives, many patients have already tried a familiar set of recommendations, but still don’t feel meaningfully better. More water. More salt. Compression stockings. Cardio. One medication, then another. Even when parts of the plan help, it can still feel like you’re managing symptoms all day instead of getting your life back.
These foundational strategies do have a role. Increasing fluids and salt can help expand blood volume and support circulation. Compression garments can help reduce pooling in the lower body. And graded exercise, when introduced carefully and progressed slowly, may improve tolerance over time.2-4
The challenge is that POTS is rarely only about circulation or a single number on a chart. It involves broader autonomic nervous system dysregulation. When care focuses only on heart rate or blood pressure, it may miss other drivers of daily impairment, including fatigue, digestive symptoms, cognitive fog, and the stress of living in a body that feels unpredictable.
Medications Can Help, But They’re Not Always Enough
Some people benefit from medications such as beta blockers, which can reduce heart rate, or midodrine, which supports blood vessel tone and blood pressure.1 These options can be useful, particularly when tachycardia or low blood pressure is a major part of the symptom picture. At the same time, responses vary, and side effects like fatigue, mood changes, or gastrointestinal upset can limit how well a medication fits over the long term.
Dr. Philip Fischer, a pediatrician at Mayo Clinic who treats adolescents with POTS, has noted that even when medication is part of the plan, it rarely addresses every symptom on its own.1 For many patients, what’s most discouraging is not trying treatment, but trying it without a clear framework for reassessment, adjustment, and support over time.
One-Size-Fits-All Doesn’t Work for POTS
What helps one person may not help another, and that’s not a failure on your part. POTS can present differently from person to person, and it is often connected with other conditions, including hypermobility disorders, autoimmune issues, and post-viral syndromes.2 That means a treatment plan focused only on cardiovascular metrics may overlook contributing factors that shape how symptoms show up day to day.
Many people describe feeling like they’re “patching holes” rather than building a plan that fits their body. They’re given broad recommendations and left to figure out pacing, flare management, and follow-through without enough guidance or personalization.
It’s understandable that many patients explore complementary therapies, not out of desperation, but because they want care that considers the whole person and adapts as their needs change.
A More Holistic Path to Managing POTS Symptoms
If you’ve tried common recommendations, like increased salt and fluids, medications, and structured exercise plans, and still feel limited by symptoms, you’re not alone. Many people with POTS reach a point where they’re following the guidance they’ve been given, but day-to-day function still feels unstable.
At Nyberg Acupuncture & Wellness, we often see a similar pattern of nervous system dysregulation in patients living with conditions like fibromyalgia and complex chronic fatigue, where dizziness, brain fog, and post-exertional crashes may show up differently depending on the diagnosis. What these experiences can share is the feeling of not being able to rely on your body. That’s often where care needs to start.
A more integrated, whole-person approach can be helpful when symptoms are complex, overlapping, or slow to improve.
At Nyberg Acupuncture & Wellness in Tualatin, care is structured and personalized. We start with a detailed intake, look for contributing factors that may be shaping your symptoms, and adjust the plan over time based on how you respond.
Supporting the Nervous System, Not Just the Heart
POTS is fundamentally a disorder of nervous system regulation. That’s why an important focus of care is supporting the autonomic nervous system, which influences heart rate, digestion, blood pressure, and other essential functions.
One of the key pathways involved is the vagus nerve, a major communication channel between the brain and body that plays a role in heart rate regulation, digestion, and the body’s recovery response. When vagal signaling is disrupted, symptoms like dizziness, nausea, and exhaustion can be harder to stabilize.
Acupuncture has been studied for its effects on autonomic regulation. Research suggests it may reduce markers associated with sympathetic activation (the “fight-or-flight” response) and influence heart rate variability, a physiologic measure often used as a proxy for nervous system resilience.5
In a 2015 multicenter clinical trial, patients with chronic fatigue who received acupuncture reported improvements in fatigue-related outcomes and overall well-being, without medication-related side effects.6 While chronic fatigue is not the same diagnosis as POTS, the symptom overlap is meaningful, especially for patients dealing with persistent exhaustion and limited recovery.
Other research suggests acupuncture may support symptoms such as brain fog, anxiety, and autonomic dysfunction, in part through its effects on heart rate variability and autonomic balance.7 For many patients with POTS, cognitive clarity and emotional steadiness are as important as physical stability.
Functional MRI research also suggests acupuncture can influence brain structures involved in autonomic regulation, including the amygdala, hypothalamus, and regions of the brainstem that interact with vagal pathways.8 This type of central nervous system involvement may help explain why some people report broader changes in symptoms over time, beyond heart rate alone.
Digestive Symptoms and POTS
If POTS leaves your stomach in knots with bloating, nausea, cramping, or constipation, you’re not imagining it. Digestive symptoms are common in POTS and may relate to changes in autonomic regulation that affect gut motility and circulation.
Acupuncture has also been studied for digestive symptom support. A 2021 systematic review of 61 randomized controlled trials found that acupuncture improved symptoms of functional gastrointestinal disorders, including irritable bowel syndrome and functional dyspepsia.9 In that analysis, acupuncture was also associated with fewer side effects than some medication comparators.9
More Than One Modality, Working Together
While acupuncture forms the foundation of care, Nyberg Acupuncture & Wellness may incorporate additional, noninvasive therapies when symptoms are complex or overlapping. These services are selected based on your symptom pattern and adjusted over time based on response.
- ATP Resonance BioTherapy® uses gentle electrical currents to support tissue-level regulation and systemic balance. This may be especially useful for patients also managing chronic pain, fatigue, or stress-related dysregulation.
- O3 ReBoot Therapy® may be considered for patients dealing with brain fog, digestive discomfort, or inflammatory symptoms. It is used as a supportive therapy alongside acupuncture, with the goal of improving overall physiologic recovery.
Rather than a one-size-fits-all protocol, care is delivered in a structured way with ongoing reassessment. The goal is to support more stable day-to-day function, not to promise immediate or uniform results.
We don’t treat the diagnosis in isolation. We treat the person living with it, with careful evaluation, clear planning, and therapies chosen to match your needs.
You’re Not Making It Up, and You Don’t Have to Manage It Alone
Living with POTS can feel like you’re constantly defending your experience to doctors, to loved ones, and sometimes even to yourself.
You may have been told it’s anxiety. That it’s “not that bad.” That you just need more sleep, less stress, or more willpower. But that doesn’t explain why your heart races when you stand, why your thinking feels slower or scattered, or why your body seems to need more recovery than movement.
You deserve to be taken seriously. You deserve care that looks beyond numbers on a chart and considers the full picture of what you’re experiencing.
At Nyberg Acupuncture & Wellness, we understand that POTS is rarely just one symptom. It can affect confidence, independence, and peace of mind over time. Our approach is designed to support the nervous system with individualized care and a treatment plan that can be adjusted based on your response.
Whether you’re newly diagnosed, years into your search for answers, or still trying to understand what’s happening in your body, you don’t have to navigate it alone.
Dr. Jeffrey Savage, LAc, DACM offers individualized consultations to review your history, current symptoms, and prior treatments, and to determine whether acupuncture and supportive therapies may be a good fit. If you’re a candidate, we’ll outline a clear plan based on your needs and goals. Learn more about our approach and philosophy here.
Frequently Asked Questions about POTS and Acupuncture
-
Acupuncture may help support autonomic nervous system regulation, which is often affected in POTS. Some patients report changes in symptoms like dizziness, fatigue, and brain fog when acupuncture is part of a whole-person care plan.
-
Natural approaches often include increasing hydration and salt intake (when appropriate), using compression garments, building gentle movement over time, and prioritizing pacing and recovery. Some people also explore acupuncture and other supportive therapies aimed at nervous system regulation, along with stress management and digestive support.
-
When performed by a licensed provider who has experience working with dysautonomia, acupuncture is generally considered safe. At Nyberg Acupuncture & Wellness, treatments are adjusted to your tolerance, with the goal of supporting steadier regulation without provoking symptoms.
-
Some patients report fewer or less intense dizzy episodes over time with acupuncture, especially when care is coordinated with foundational strategies like hydration, compression, and paced activity. Results vary depending on contributing factors and overall symptom pattern.
-
Medications can be helpful for some patients, but symptoms may still persist. Acupuncture and complementary therapies may be considered as supportive options for areas that are often harder to stabilize, such as fatigue, brain fog, digestive symptoms, and post-exertional crashes.
-
Nyberg Acupuncture & Wellness is located in Tualatin and serves the greater Portland area. The best way to get started is to call +1 (503) 336-4747 to request a consultation and discuss whether this approach may be a good fit. If you cannot call right away, you can fill out this form and our team will follow up.
Ready to Take the First Step?
The best way to get started is to call us directly at +1 (503) 336-4747.
If you prefer, you can also schedule a consultation with Dr. Savage. We welcome patients from Tualatin and the greater Portland area, and we’ll take the time to understand your symptoms and discuss next steps.
If you’re ready for a clearer plan and more support, we’re here to help.
References:
- Fischer P. Understanding POTS: Mayo Clinic explains symptoms and treatment. Mayo Clinic. Published January 29, 2009. Accessed May 18, 2025. https://www.youtube.com/watch?v=iJ9bv7jx-Ls
- Zhao S, Tran VH. Postural Orthostatic Tachycardia Syndrome. [Updated 2023 Aug 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. Available from: https://www.ncbi.nlm.nih.gov/books/NBK541074/
- Raj SR, Bourne KM, Stiles LE, et al. Postural orthostatic tachycardia syndrome (POTS): Priorities for POTS care and research from a 2019 National Institutes of Health Expert Consensus Meeting - Part 2. Auton Neurosci. 2021;235:102836. doi:10.1016/j.autneu.2021.102836
- Cleveland Clinic. Postural Orthostatic Tachycardia Syndrome (POTS). Updated 2024. Accessed May 18, 2025. https://my.clevelandclinic.org/departments/neurological/depts/neuromuscular/postural-orthostatic-tachycardia-syndrome
- Chung JW, Yan VC, Zhang H. Effect of acupuncture on heart rate variability: a systematic review. Evid Based Complement Alternat Med. 2014;2014:819871. doi:10.1155/2014/819871
- Kim JE, Seo BK, Choi JB, et al. Acupuncture for chronic fatigue syndrome and idiopathic chronic fatigue: a multicenter, nonblinded, randomized controlled trial. Trials. 2015;16:314. doi:10.1186/s13063-015-0857-0
- Martínez OM, Fossion R, Piceno YG, et al. Heart rate variability and psychometric analysis in patients with hyperactive heart fire syndrome. J Acupunct Meridian Stud. 2021;14(4):137–148. doi:10.51507/j.jams.2021.14.4.137
- Hui KK, Marina O, Liu J, Rosen BR, Kwong KK. Acupuncture, the limbic system, and the anticorrelated networks of the brain. Auton Neurosci. 2010;157(1-2):81–90. doi:10.1016/j.autneu.2010.03.022
- Wang XY, Wang H, Guan YY, et al. Acupuncture for functional gastrointestinal disorders: a systematic review and meta-analysis. J Gastroenterol Hepatol. 2021;36(11):3015–3026. doi:10.1111/jgh.15645