Hope for Crohn’s Disease: The Healing Power of Acupuncture
Crohn’s disease can become an ongoing, exhausting cycle of flare-ups, partial improvement, and recurrence. With over 3 million people in the U.S. diagnosed with inflammatory bowel disease (IBD), including Crohn’s disease and ulcerative colitis1, many continue to live with persistent abdominal pain, digestive instability, fatigue, and the uncertainty that comes with an unpredictable condition.
When symptoms remain active despite conventional care, it often signals the need for a more individualized and structured approach. Rather than focusing only on short-term symptom suppression, long-term management requires evaluating contributing factors, monitoring response over time, and adjusting care accordingly.
Acupuncture for Crohn’s disease offers a non-invasive option that supports inflammatory regulation, digestive function, and overall resilience when used within a structured treatment plan. As part of a broader inflammatory bowel disease treatment plan, acupuncture can be integrated thoughtfully for patients seeking steady, medically informed care.
Common Crohn’s Disease Symptoms and Flare Patterns
Crohn’s disease rarely presents the same way in every patient. Symptoms may fluctuate in intensity, improve temporarily, or return without clear warning. Over time, this unpredictability can interfere with work, relationships, nutrition, and overall stability.
Common Crohn’s disease symptoms include:
- Abdominal Pain and Cramping: Ongoing discomfort or sharp pain often reflects active inflammation within the digestive tract.
- Diarrhea: Frequent or urgent bowel movements may disrupt daily routines and contribute to dehydration or nutrient loss.
- Fatigue: Persistent inflammation and impaired nutrient absorption can leave you feeling depleted, even with adequate rest.
- Unintended Weight Loss: Difficulty absorbing nutrients may lead to weight changes and reduced physical resilience.
- Fever During Flares: Low-grade or intermittent fever can signal increased inflammatory activity.
- Mouth Sores: Painful oral ulcers may accompany gastrointestinal inflammation.
Beyond the physical symptoms, many patients describe the mental strain of not knowing when the next flare will occur. Planning becomes difficult. Social events require strategy. Even periods of improvement may feel uncertain.
When symptoms persist or repeatedly return, it often indicates the need for a more structured treatment approach rather than reactive symptom management alone. Identifying patterns, contributing triggers, and inflammatory drivers is a critical step in developing an effective Crohn’s treatment plan.
What Contributes to Crohn’s Disease and IBD?
The exact cause of inflammatory bowel disease (IBD), including Crohn’s disease, is not fully understood. Most researchers agree that Crohn’s develops from a combination of interacting factors rather than a single trigger. Understanding these contributors helps guide a more precise and individualized treatment approach.
Key contributing factors may include:
- Genetic Predisposition: A family history of IBD can increase susceptibility. Certain genetic markers are associated with immune dysregulation and inflammatory responses in the gastrointestinal tract.
- Immune System Dysregulation: In Crohn’s disease, the immune system may overreact to normal gut stimuli, mistakenly attacking healthy intestinal tissue and sustaining chronic inflammation.
- Environmental Influences: Diet, chronic stress, infections, and environmental exposures may influence inflammatory activity or trigger flare patterns in susceptible individuals.
- Gut Microbiome Imbalance: Alterations in the composition of intestinal bacteria have been linked to changes in immune signaling and intestinal barrier integrity.
- Lifestyle Factors: Smoking, inadequate nutrition, and prolonged stress can worsen inflammatory activity and increase flare frequency.
For many patients, symptoms persist because multiple contributing factors interact simultaneously. Effective Crohn’s treatment options often require identifying patterns, evaluating inflammatory drivers, and adjusting care as the condition evolves rather than relying on a single intervention.
How Acupuncture May Support Crohn’s Disease and IBD
Acupuncture is not a replacement for conventional Crohn’s treatment options, but it may serve as a structured, non-invasive addition to a comprehensive inflammatory bowel disease treatment plan. Research suggests it may influence inflammatory signaling, digestive regulation, and stress response when applied consistently and monitored over time.
- Symptom Relief: Many patients experience abdominal pain and cramping related to visceral hypersensitivity and ongoing inflammation. Acupuncture has been shown to help regulate gut motility and sensory signaling, which may reduce discomfort and improve day-to-day stability.2,3
- Reduced Inflammation: Studies indicate that acupuncture may lower pro-inflammatory cytokines such as TNF-alpha, which are known to play a role in Crohn’s disease activity. Modulating inflammatory signaling may contribute to fewer or less intense flare patterns.4,5
- Improved Digestive Function: Research has demonstrated improvements in intestinal barrier function and gut microbiota composition in patients receiving acupuncture. These changes may support more consistent digestive function and symptom control.4,2
- Stress and Mood Regulation: Chronic inflammatory conditions often carry a psychological burden. Evidence suggests acupuncture may reduce anxiety and depressive symptoms in individuals with Crohn’s disease, supporting overall resilience during long-term care.3
- Support for Ongoing Disease Management: Some studies indicate that acupuncture and moxibustion may help maintain lower disease activity scores over time when used as part of continued care. This supports its role in structured, longitudinal management rather than short-term symptom suppression.5,4
Individualized Crohn’s Disease Care
Living with Crohn’s disease often requires more than standardized treatment protocols. When symptoms persist, care must adapt to the individual rather than the diagnosis alone.
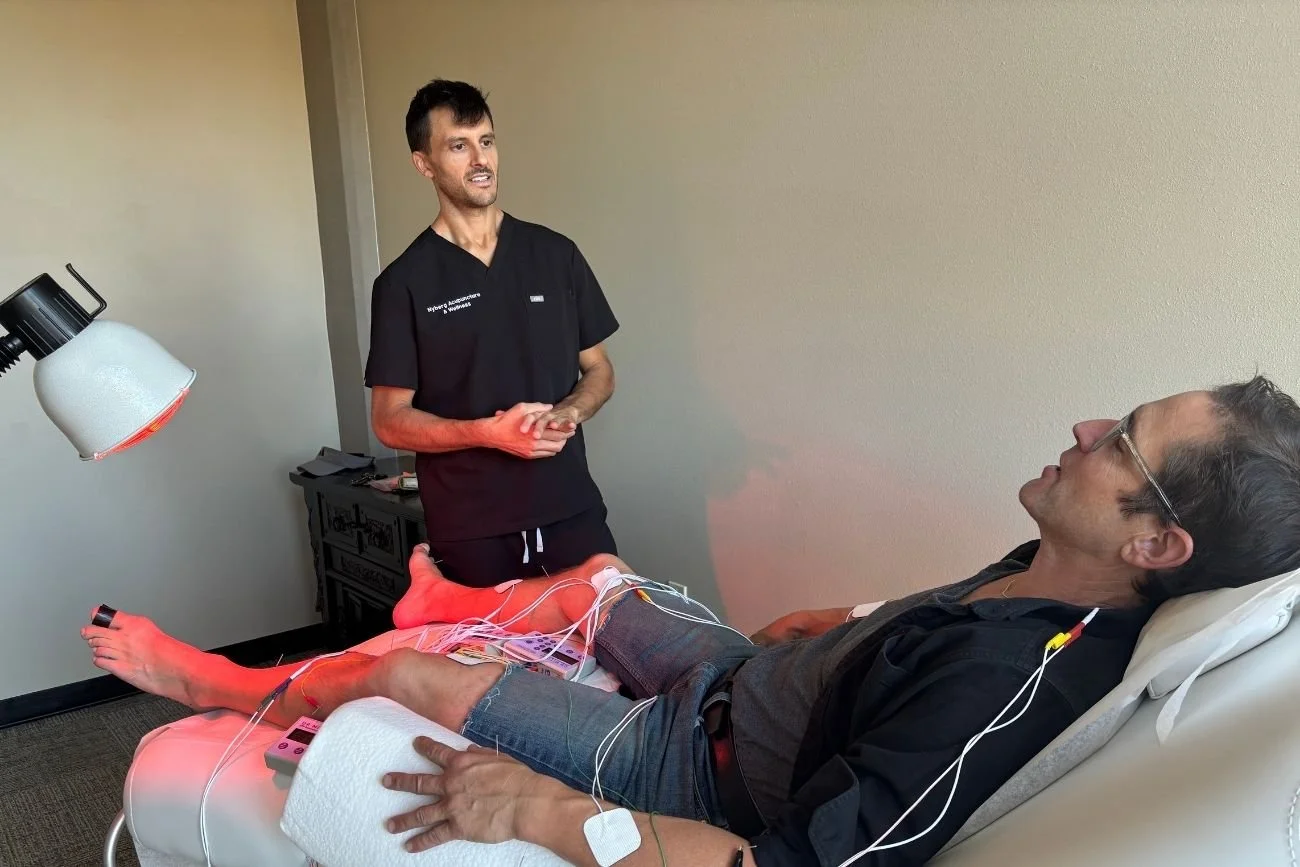
At Nyberg Acupuncture & Wellness, we design personalized treatment plans based on your symptom history, inflammatory patterns, digestive function, and prior interventions. Dr. Savage evaluates these factors to determine how acupuncture for Crohn’s disease and supportive therapies may fit into your broader care plan.
When appropriate, we integrate modern therapies such as ATP Resonance BioTherapy® to support tissue recovery and inflammatory regulation. Our goal is not temporary symptom suppression, but steady and measurable progress.
A Structured Approach to Crohn’s Disease Treatment
Crohn’s disease rarely improves with symptom-based care alone. When flare patterns continue or conventional strategies provide incomplete relief, treatment must become more individualized and responsive.
At Nyberg Acupuncture & Wellness, we begin with a detailed evaluation of your symptom history, flare frequency, inflammatory patterns, digestive function, and prior interventions. Dr. Savage uses this information to design a personalized plan and adjusts it over time based on how your body responds.
We may incorporate acupuncture to support inflammatory regulation, digestive stability, and nervous system balance. When clinically appropriate, we also integrate modern supportive therapies such as ATP Resonance BioTherapy ®, which targets specific tissues to promote cellular repair and recovery.
Crohn’s disease treatment follows the same structured model we use for other chronic and complex conditions, where ongoing assessment guides thoughtful treatment adjustments rather than one-time intervention.
Care remains focused on measurable progress, clinical oversight, and steady long-term improvement under the direction of Dr. Jeffrey Savage, LAc, DACM.
When You’re Ready to Begin Care
Crohn’s disease can narrow your world over time. Care should help expand it again.
If your symptoms continue despite prior treatment, the next step is a structured evaluation. During your consultation, Dr. Savage will review your symptom history, flare frequency, prior interventions, and overall health patterns. He will then determine whether acupuncture for Crohn’s disease or additional supportive therapies may fit into your broader inflammatory bowel disease treatment plan.
To begin, call us directly at +1 (503) 336-4747. Our team will answer your questions and help coordinate next steps.
If you prefer, you may also submit your information through our consultation request page, and we will contact you to discuss scheduling.
For additional insight into how we approach chronic digestive and inflammatory conditions, you can explore our blog.
Care begins with clarity. The first step is a thoughtful evaluation.
Frequently Asked Questions About Acupuncture for Crohn’s Disease and IBD
-
Yes, when performed by a licensed practitioner, acupuncture is generally considered safe for individuals with Crohn’s disease. Care must be tailored to your current disease activity, overall health status, and medical history. A structured evaluation determines whether acupuncture is appropriate for you.
-
No. Acupuncture does not replace prescribed Crohn’s medications. You should continue to follow your prescribing physician’s instructions regarding all medications unless your doctor advises otherwise. Acupuncture is typically used as part of a comprehensive inflammatory bowel disease treatment plan alongside gastroenterology care, with the goal of integration rather than substitution.
-
Research suggests acupuncture may help regulate inflammatory signaling, gut motility, stress response, and intestinal barrier function. These mechanisms may support symptom stability and reduced disease activity when used consistently within a structured treatment plan.
-
Some studies indicate acupuncture may reduce pro-inflammatory cytokines such as TNF-alpha, which play a role in Crohn’s disease activity. Lower inflammatory signaling may contribute to improved symptom control over time.
-
The number of sessions depends on symptom severity, flare frequency, and response to care. Chronic inflammatory conditions require a series of treatments with periodic reassessment rather than a single visit.
-
Acupuncture may support symptom regulation during milder flare activity. However, treatment decisions depend on severity and overall medical stability. Evaluation helps determine timing and treatment intensity.
-
We begin with a detailed evaluation and build a personalized treatment plan that evolves based on your response. Rather than using standardized protocols, we adjust care according to inflammatory patterns, digestive function, and long-term goals. When clinically appropriate, we integrate supportive therapies such as ATP Resonance BioTherapy® and O3 ReBoot Therapy® to complement acupuncture and address tissue recovery, inflammatory regulation, and systemic stress.
References:
- CDC. IBD Facts and Stats. Inflammatory bowel disease (IBD). July 22, 2024. Accessed October 6, 2024. https://www.cdc.gov/inflammatory-bowel-disease/php/facts-stats/index.html
- Song G, Fiocchi C, Achkar JP. Acupuncture in Inflammatory Bowel Disease. Inflamm Bowel Dis. 2019;25(7):1129-1139. doi:10.1093/ibd/izy371
- Bae JH, Kang SY, You SE, Jeong HI, Jang S, Kim KH. The Effects of Acupuncture on Crohn's Disease: a systematic review and meta-analysis. J Pharmacopuncture. 2023;26(3):211-226. doi:10.3831/KPI.2023.26.3.211
- Bao C, Wu L, Wang D, et al. Acupuncture improves the symptoms, intestinal microbiota, and inflammation of patients with mild to moderate Crohn's disease: A randomized controlled trial. EClinicalMedicine. 2022;45:101300. Published 2022 Feb 12. doi:10.1016/j.eclinm.2022.101300
- Bao CH, Zhao JM, Liu HR, et al. Randomized controlled trial: moxibustion and acupuncture for the treatment of Crohn's disease. World J Gastroenterol. 2014;20(31):11000-11011. doi:10.3748/wjg.v20.i31.11000