Acupuncture for Fibromyalgia Pain and Chronic Symptoms
Fibromyalgia can wear you down over time. The pain lingers, the fatigue doesn’t lift, and sleep rarely feels restorative. Many people reach a point where they’ve tried medications, physical therapy, or other treatments, yet the symptoms keep coming back or never fully improve.
At that stage, care needs to shift. Acupuncture for fibromyalgia allows us to work directly with the patterns behind your pain, fatigue, and sleep disruption. Instead of reacting to symptoms as they appear, treatment follows a structured plan that stays consistent while adapting to how your body responds.
Fibromyalgia doesn’t follow a predictable pattern. Symptoms can move, intensify, or ease without warning, and what drives them often changes from day to day. That variability is exactly why treatment needs to stay steady and intentional, rather than chasing each new flare-up.
In the sections below, we’ll walk through the common causes and contributing factors behind fibromyalgia, the symptoms it can create throughout the body, and how acupuncture fits into a comprehensive fibromyalgia treatment plan.
Understanding Fibromyalgia Causes and Contributing Factors
Fibromyalgia is a complex condition, and no single cause explains why symptoms develop or persist. Instead, fibromyalgia tends to involve multiple contributing factors that affect how the body processes pain, responds to stress, and recovers over time. This is one reason fibromyalgia treatment requires a structured, individualized approach rather than a one-size solution.
Genetic Factors
Genetics can influence susceptibility to fibromyalgia. Research shows it often runs in families, and individuals with a family history may have a higher risk of developing the condition.1 These genetic factors can affect how the nervous system processes pain and how the body responds to physical and emotional stress.
Environmental Triggers
Fibromyalgia symptoms often begin or worsen after a triggering event. Physical injury, illness, infection, or prolonged stress can disrupt normal pain processing and lead to persistent symptoms. In many cases, these triggers do not resolve cleanly, which can leave the nervous system in a heightened, reactive state.
Lifestyle Factors
Daily habits can influence how fibromyalgia symptoms present and progress. Poor sleep, limited physical activity, and ongoing stress can all amplify pain and fatigue. While lifestyle changes alone are rarely enough to resolve symptoms, they play an important role in how well the body responds to treatment over time.
Hormonal Imbalances
Hormonal shifts may affect symptom severity, particularly in how the body regulates pain and energy. Changes in thyroid function or sex hormones such as estrogen can influence how symptoms fluctuate. Fibromyalgia is more common in women, suggesting a hormonal component in how the condition develops and presents.
Immune System Dysfunction
Some evidence suggests that altered immune responses and inflammatory processes may contribute to fibromyalgia symptoms.2 When the immune system does not regulate properly, it may increase sensitivity to pain and contribute to ongoing fatigue.
Because fibromyalgia involves multiple systems, identifying these contributing factors helps guide treatment. Instead of focusing on a single cause, care often needs to address patterns over time, allowing treatment to stay consistent while adapting to how your body responds.
Common Fibromyalgia Symptoms and How They Affect Daily Life
Fibromyalgia presents with a wide range of symptoms that can shift over time and affect multiple systems. While each person’s experience is different, most patients deal with a combination of persistent pain, fatigue, and cognitive strain that affects daily function. Recognizing how these symptoms show up is an important step in building an effective fibromyalgia treatment plan.
Widespread Pain
Widespread pain is one of the defining features of fibromyalgia. It often presents as a deep, aching discomfort but can also feel sharp or throbbing. Pain may move from one area of the body to another, which can make it difficult to identify a clear source.
Low Back Pain & Sciatica: Ongoing low back pain is common and may extend into the legs as sciatica. This can limit movement, interfere with daily tasks, and contribute to overall physical strain.
Neck Pain: Neck pain and stiffness frequently occur alongside fibromyalgia. Limited range of motion and muscle tension in this area can also contribute to headaches and upper body discomfort.
Headaches and Migraines
Frequent headaches and migraines are common in fibromyalgia. These episodes can range in intensity and often interfere with focus, work, and routine activities.
Heel Pain and Plantar Fasciitis
Heel pain, including plantar fasciitis, may develop due to increased sensitivity in connective tissues. Pain is often worse in the morning or after periods of inactivity, making walking or standing more difficult.
Chronic Fatigue
Chronic fatigue is a central component of fibromyalgia. This type of fatigue does not improve with rest and can make even basic activities feel demanding. Many patients describe feeling drained despite adequate sleep.
Mood Changes
Ongoing pain and fatigue can affect mental and emotional health. Some patients experience depression, reduced motivation, or a sense of withdrawal from activities they once enjoyed. These changes often develop gradually as symptoms persist.
Roaming Body Pain
Fibromyalgia pain does not always stay in one location. It can shift throughout the body, sometimes daily. This unpredictability makes symptoms harder to manage and can create a sense of instability in how the body feels from one day to the next.
Additional Symptoms
Other symptoms that may accompany fibromyalgia include:
- Sleep Disturbances: Difficulty falling or staying asleep, often leading to unrefreshing rest.
- Cognitive Issues: Often referred to as "fibro fog," this includes difficulty with memory, focus, and mental clarity.
- Sensitivity to Touch: Increased sensitivity to pressure, temperature changes, and physical contact.
Fibromyalgia symptoms rarely exist in isolation. They tend to overlap and reinforce each other over time, which is why treatment needs to address patterns across the body rather than focusing on a single symptom.
How Acupuncture Fits Into Fibromyalgia Treatment
Acupuncture plays a central role in how we approach fibromyalgia treatment, especially for patients seeking structured fibromyalgia pain treatment without relying solely on medication. Rather than addressing symptoms in isolation, acupuncture allows us to work with the underlying patterns that drive chronic symptoms over time.
Fibromyalgia often behaves like a chronic pain condition involving the nervous system, circulation, and muscular tension. Because of this, treatment needs to be consistent and structured, not reactive. Acupuncture provides a way to influence these systems directly while allowing care to adapt based on how your body responds.
How Acupuncture Works
Acupuncture stimulates specific points to influence pain signaling, circulation, and muscle function. This process supports several key mechanisms:
- Regulating Pain Pathways: Acupuncture encourages the release of endorphins and helps modulate how the nervous system processes pain, which can reduce overall pain sensitivity.
- Improving Circulation: Increased blood flow supports tissue health, reduces inflammation, and helps the body recover more efficiently.
- Reducing Muscle Tension: By relaxing tight or reactive muscles, acupuncture can improve mobility and decrease physical strain.
These effects are not isolated. Over time, they build on each other, which is why consistency in treatment plays a critical role in progress.
How Treatment Is Applied in Fibromyalgia
Fibromyalgia symptoms can shift from day to day, but treatment should not chase each individual flare-up. Instead, care follows a structured plan that targets the broader patterns contributing to pain, fatigue, and dysfunction.
At our clinic, acupuncture is part of a personalized treatment plan that evolves over time. We assess how your symptoms present, how long they’ve been present, and how your body responds to care. Based on that, treatment is adjusted while still maintaining consistency.
This approach allows us to gradually reduce symptom intensity, improve stability, and support more predictable progress.
Potential Benefits of Acupuncture for Fibromyalgia Pain
When applied within a structured plan, acupuncture may support:
- Reduced Pain and Stiffness: By improving circulation and regulating pain pathways, treatment can help decrease widespread discomfort.
- Improved Sleep Quality: Better sleep supports recovery and can reduce the severity of fatigue.
- Increased Energy Levels: As sleep and pain improve, many patients notice more consistent energy throughout the day.
- Improved Mental Clarity: Reducing pain and fatigue can help alleviate cognitive symptoms such as fibro fog.
- Support for Mood Regulation: Calming the nervous system may help reduce stress, anxiety, and emotional strain associated with chronic symptoms.
- Digestive Support: In some cases, treatment may help regulate digestive function, which can be affected in fibromyalgia.
These changes often develop gradually as treatment builds over time.
Integrating Acupuncture with Other Therapies
Acupuncture is most effective when used as part of a comprehensive treatment plan. In our clinic, we often integrate therapies such as ATP Resonance BioTherapy ® and O3 ReBoot Therapy ® based on each patient’s presentation.
These therapies are not added arbitrarily. They are selected to complement acupuncture and support the same treatment goals, whether that involves improving circulation, reducing inflammation, or supporting recovery.
You can explore our fibromyalgia treatment page to see how these therapies work together to support long-term improvement.
If fatigue and sleep disruption are primary concerns, our post on acupuncture for fibromyalgia fatigue takes a deeper look at how treatment can support energy and rest.
Frequently Asked Questions About Acupuncture for Fibromyalgia Pain
-
Acupuncture for fibromyalgia may help reduce widespread pain, stiffness, fatigue, sleep disturbances, anxiety, and cognitive symptoms such as brain fog. Treatment focuses on improving how the body regulates pain and recovers over time rather than targeting one symptom in isolation.
-
Yes. Acupuncture is a non-pharmaceutical, non-invasive approach to fibromyalgia treatment. It works by supporting the body’s natural regulatory systems, making it a suitable option for patients looking to avoid or reduce reliance on medications.
-
The number of sessions depends on symptom severity, duration, and how your body responds to care. Fibromyalgia is typically managed through a structured treatment plan that emphasizes consistency, with adjustments made over time based on progress.
-
Yes, many patients seek acupuncture for chronic fatigue in fibromyalgia and ongoing sleep disruption. By supporting nervous system regulation and improving sleep quality, treatment can help restore more consistent energy levels over time.
-
Acupuncture is often used as part of a long-term fibromyalgia pain treatment strategy. Rather than providing temporary relief alone, it can help regulate pain pathways and improve function when applied consistently within a personalized treatment plan.
-
Yes. In our clinic, acupuncture is often combined with therapies such as ATP Resonance BioTherapy® and O3 ReBoot Therapy® when appropriate. These are integrated into a personalized plan to support circulation, recovery, and overall symptom management.
-
Many patients consider acupuncture after trying medications, physical therapy, or other approaches without lasting improvement. It may be appropriate when symptoms remain persistent, fluctuate frequently, or begin to interfere with daily function.
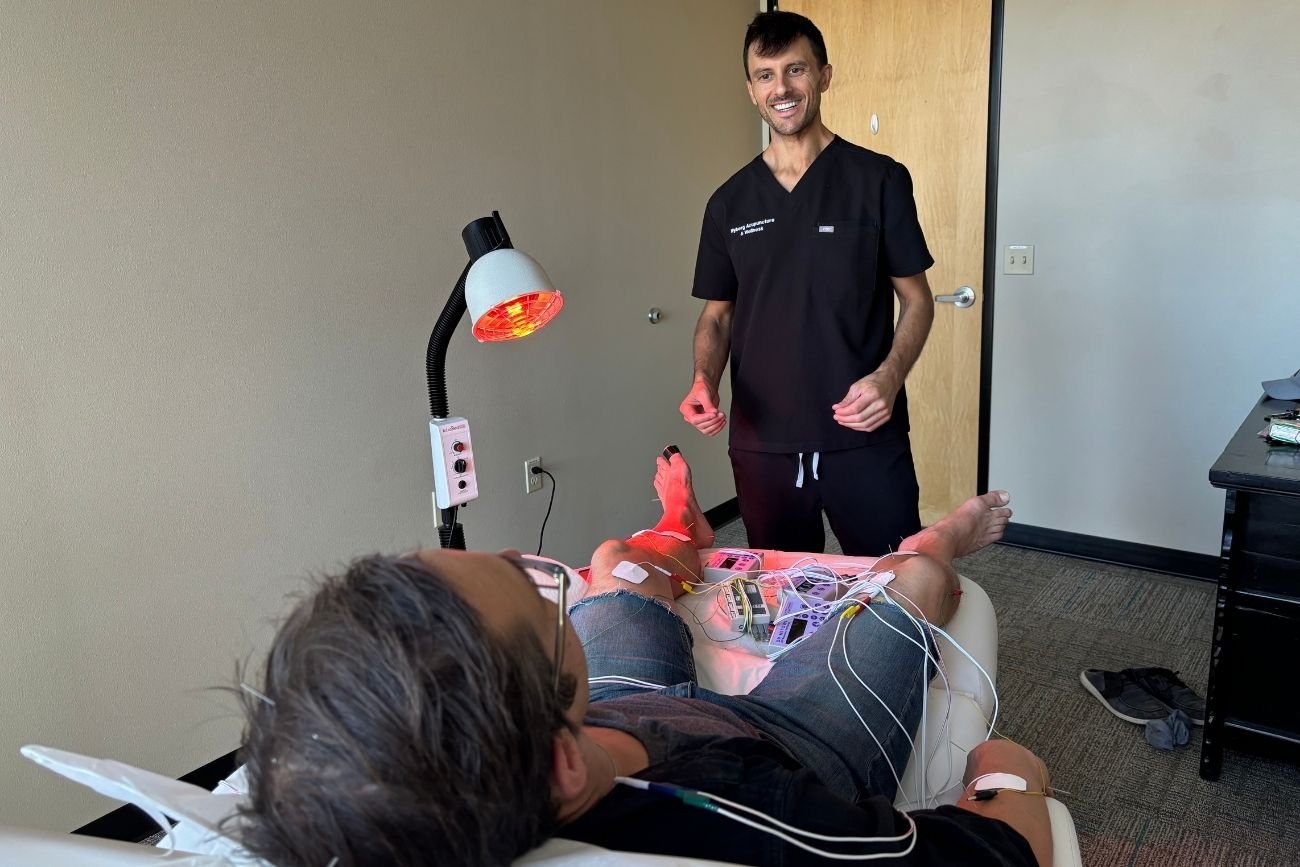
Starting Fibromyalgia Treatment at Nyberg Acupuncture & Wellness
When fibromyalgia symptoms persist despite medications, physical therapy, or other conventional care, it becomes important to step back and evaluate the full picture. A consultation with Dr. Jeffrey Savage, LAc, DACM gives us the opportunity to evaluate your symptoms, review what you’ve already tried, and determine whether acupuncture and supportive therapies are appropriate for your case.
What to Expect From Your Consultation
Fibromyalgia rarely follows a simple pattern. Pain, fatigue, sleep disruption, and cognitive symptoms can shift over time, which is why treatment needs to begin with a careful evaluation.
During your consultation, Dr. Savage will review your symptom history, the duration and pattern of your symptoms, and the factors that may be contributing to flare-ups or ongoing dysfunction. From there, we develop a personalized treatment plan based on your presentation, treatment history, and response over time.
When appropriate, treatment may also incorporate supportive therapies such as ATP Resonance BioTherapy ® and O3 ReBoot Therapy ®. These therapies are selected intentionally and used in coordination with acupuncture to support the broader goals of your care plan.
Why This Approach Matters
Fibromyalgia treatment works best when it stays structured and consistent. Rather than reacting to each symptom as it appears, we focus on the larger patterns driving pain, fatigue, and instability. That approach allows treatment to stay grounded while still adapting as your body responds.
Our goal is to help you move toward more stable function, better symptom control, and a clearer path forward.
Take the First Step
The best way to get started is to call us directly at +1 (503) 336-4747.
If you prefer, you can also schedule a consultation through our web form. We welcome patients from Tualatin and the greater Portland area and take the time to understand your symptoms and outline clear next steps.
You can also explore other conditions we treat to better understand how our clinic approaches chronic pain and ongoing symptoms.
References:
- Arnold LM, Hudson JI, Hess EV, et al. Family study of fibromyalgia. Arthritis Rheum. 2004;50(3):944-952. doi:10.1002/art.20042
- Gur A, Oktayoglu P. Status of immune mediators in fibromyalgia. Current Pain and Headache Reports. 2008;12(3):175-181. doi:10.1007/s11916-008-0031-4